Hudson County Public Health Profile Report
Asthma Prevalence in Adults: Estimated Percent (Age-adjusted), 2017-2020*
Hudson 7.7%95% Confidence Interval (5.9% - 10.1%)Description of the Confidence IntervalThe confidence interval indicates the range of probable true values for the level of risk in the community.
A value of "NA" (Not Available) will appear if the confidence interval was not published with the NJSHAD indicator data for this measure.State 8.5%U.S. NA NA=Data not available.Hudson Compared to State
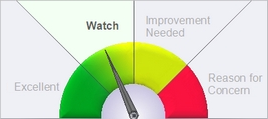
Description of GaugeDescription of the Gauge
This graphic is based on the county data to the left. It compares the county value of this indicator to the state overall value.- Excellent = The county's value on this indicator is BETTER than the state value, and the difference IS statistically significant.
- Watch = The county's value is BETTER than state value, but the difference IS NOT statistically significant.
- Improvement Needed = The county's value on this indicator is WORSE than the state value, but the difference IS NOT statistically significant.
- Reason for Concern = The county's value on this indicator is WORSE than the state value, and the difference IS statistically significant.
The county value is considered statistically significantly different from the state value if the state value is outside the range of the county's 95% confidence interval. If the county's data or 95% confidence interval information is not available, a blank gauge image will be displayed with the message, "missing information."NOTE: The labels used on the gauge graphic are meant to describe the county's status in plain language. The placement of the gauge needle is based solely on the statistical difference between the county and state values. When selecting priority health issues to work on, a county should take into account additional factors such as how much improvement could be made, the U.S. value, the statistical stability of the county number, the severity of the health condition, and whether the difference is clinically significant.
Why Is This Important?
Asthma is a serious personal and public health issue that has far reaching medical, economic, and psychosocial implications. People with asthma are more likely to miss school or work, report feelings of depression, and experience an overall reduced quality of life. Asthma is also costly, with expenses from routine checkups, emergency department visits, hospitalizations, and medications putting a significant burden on families, the health care sector, and the economy. Though it cannot be cured, asthma can be controlled through quality health care, appropriate medications, and good self-management skills. When asthma is controlled, people with the disease have few, if any, symptoms, and can live normal and productive lives.How Are We Doing?
In 2020, the adult asthma prevalence in New Jersey was 8.7%. Blacks (12.2%) have higher prevalence of asthma compared to Whites (8.9%) and Asians (3.2%) in the state. Adult asthma prevalence is higher for women than men in every age category.What Is Being Done?
New Jersey is conducting outreach to provide asthma self-management education to reduce asthma related visits to the emergency departments for both adults and children with asthma. The NJ In-Home Asthma Program will be implemented to 1) improve asthma control; 2) improve use of routine Primary Care Provider (PCP) visits for asthma management; 3) reduce ED or Urgent Care use for uncontrolled asthma; 4) provide education and resources for reducing asthma triggers in the home; and 5) provide PCPs with updates regarding participant status and summary of asthma visit program outcomes. [https://www.nj.gov/health/fhs/chronic/asthma/in-nj/] [https://www.cdc.gov/asthma/]Evidence-based Practices
The home-based intervention is for both pediatric and adult patients with poorly controlled asthma. It is based on a staffing model that employs Community Health Workers (CHWs), with supervision by a Clinical Supervisor. It is a modified version of the NJ In-Home Asthma Pilot Project, funded by The Nicholson Foundation. The intervention is based on [https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/1939375/ Krieger's pediatric asthma care model], and is one of the interventions used by the [http://www.asthmaregionalcouncil.org/our-work/neaic/about-neaic/ New England Asthma Innovations Collaborative (NEAIC)], funded by the [https://www.usa.gov/federal-agencies/centers-for-medicare-and-medicaid-services/ Centers for Medicare and Medicaid Services]. The NJ In-Home Asthma Program includes both children and adults and will add to the literature base.Related Indicators
Relevant Population Characteristics:
Health Care System Factors:
Risk Factors:
- Obesity among High School Students in Grades 9 to 12
- Obesity Among Adults
- Cigarette Smoking Among Adults
- Number of Unhealthy Days from Carbon Monoxide, PM-10, Lead, Sulfur Dioxide, and Nitrogen Dioxide
Health Status Outcomes:
Note
All prevalence estimates are age-adjusted to the U.S. 2000 standard population (except for rates by age group). *2019 data is not included in the average estimated prevalence. No data is available for 2019Data Sources
Behavioral Risk Factor Survey, Center for Health Statistics, New Jersey Department of Health, [http://www.state.nj.us/health/chs/njbrfs/]Measure Description for Asthma Prevalence in Adults
Definition: Adults aged 18 and over, who reported having been told by a doctor that they have asthma and who currently have asthma.
Numerator: Total number of respondents answering "yes" to both of the BRFSS asthma core questions:
1. Have you ever been told by a doctor, nurse, or other health professional that you had asthma?
2. Do you still have asthma?
Denominator: Includes all survey respondents ages 18 years and older except those with missing, don't know, or refused answers to the core asthma questions

