Morris County Public Health Profile Report
Cesarean Deliveries among Low Risk Women: Percentage of Low-Risk Births, 2020
Morris 27.1%95% Confidence Interval (25.0% - 29.4%)Description of the Confidence IntervalThe confidence interval indicates the range of probable true values for the level of risk in the community.
A value of "NA" (Not Available) will appear if the confidence interval was not published with the NJSHAD indicator data for this measure.State 26.2%U.S. 25.9%Morris Compared to State
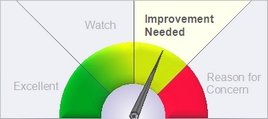
Description of GaugeDescription of the Gauge
This graphic is based on the county data to the left. It compares the county value of this indicator to the state overall value.- Excellent = The county's value on this indicator is BETTER than the state value, and the difference IS statistically significant.
- Watch = The county's value is BETTER than state value, but the difference IS NOT statistically significant.
- Improvement Needed = The county's value on this indicator is WORSE than the state value, but the difference IS NOT statistically significant.
- Reason for Concern = The county's value on this indicator is WORSE than the state value, and the difference IS statistically significant.
The county value is considered statistically significantly different from the state value if the state value is outside the range of the county's 95% confidence interval. If the county's data or 95% confidence interval information is not available, a blank gauge image will be displayed with the message, "missing information."NOTE: The labels used on the gauge graphic are meant to describe the county's status in plain language. The placement of the gauge needle is based solely on the statistical difference between the county and state values. When selecting priority health issues to work on, a county should take into account additional factors such as how much improvement could be made, the U.S. value, the statistical stability of the county number, the severity of the health condition, and whether the difference is clinically significant.
Why Is This Important?
Compared to vaginal deliveries, cesareans carry an increased risk of infection, blood clots, longer recovery, and difficulty with future pregnancies.How Are We Doing?
The cesarean delivery rate among low risk (NTSV) births declined in 2010 for the first time since the mid-1990s and in 2020 stood at 26.2%. The rate is higher among Asian (30.2%) and Black (29.9%) mothers than among Hispanic (25.8%) and White (24.4%) mothers. The Healthy New Jersey 2020 target for all low-risk mothers and for Whites, Hispanics, and Asians were achieved. If the current trend continues, the target for Blacks will also be achieved within a year or two.What Is Being Done?
In 2017, a team composed of DOH staff and external partners collaborated to develop a plan to reduce low risk c-sections in New Jersey hospitals. In 2018, DOH awarded [https://nj.gov/health/news/2018/approved/20180711a.shtml $4.7 million] to eight agencies to improve health outcomes among infants and mothers in New Jersey, including implementation of a doula pilot program to reduce the likelihood of certain birth and delivery/labor outcomes such as cesarean births. In 2021, the state [https://nj.gov/governor/news/news/562021/approved/20210202b.shtml Medicaid program began covering doula care], while also no longer paying for non-medical early elective deliveries. The same year, the [https://nurturenj.nj.gov/wp-content/uploads/2021/01/20210120-Nurture-NJ-Strategic-Plan.pdf Nurture NJ Strategic Plan] recommended that all NJ birthing hospitals meet or attain NTSV cesarean birth rates lower than the national target by instituting new, comprehensive informed consent processes for all maternity patients so that patients understand the short- and long-term risks of c-sections and the benefits of spontaneous labor for both parents and newborns. The Plan also recommended more aggressive action by state government agencies to ensure improvement, including limitations on participation in provider networks for hospitals who do not meet targets.[https://nurturenj.nj.gov/wp-content/uploads/2021/01/20210120-Nurture-NJ-Strategic-Plan.pdf#page=61 ^1^]Healthy People Objective MICH-7.1:
Reduce cesarean births among low-risk (full-term, singleton, vertex presentation) women: Women with no prior birthsU.S. Target: 24.7 percent
State Target: 27.9 percent
Related Indicators
Health Care System Factors:
Data Sources
Birth Certificate Database, Office of Vital Statistics and Registry, New Jersey Department of HealthMeasure Description for Cesarean Deliveries among Low Risk Women
Definition: The low-risk cesarean delivery rate is the percentage of cesarean deliveries among '''n'''ulliparous (first birth), '''t'''erm (37 completed weeks or more, based on the obstetric estimate), '''s'''ingleton (one fetus), '''v'''ertex (head first) births, sometimes referred to as NTSV births.
Numerator: Number of cesarean deliveries among nulliparous, full-term, singleton, vertex presentation (NTSV) births
Denominator: Total number of nulliparous, full-term, singleton, vertex presentation (NTSV) births

